





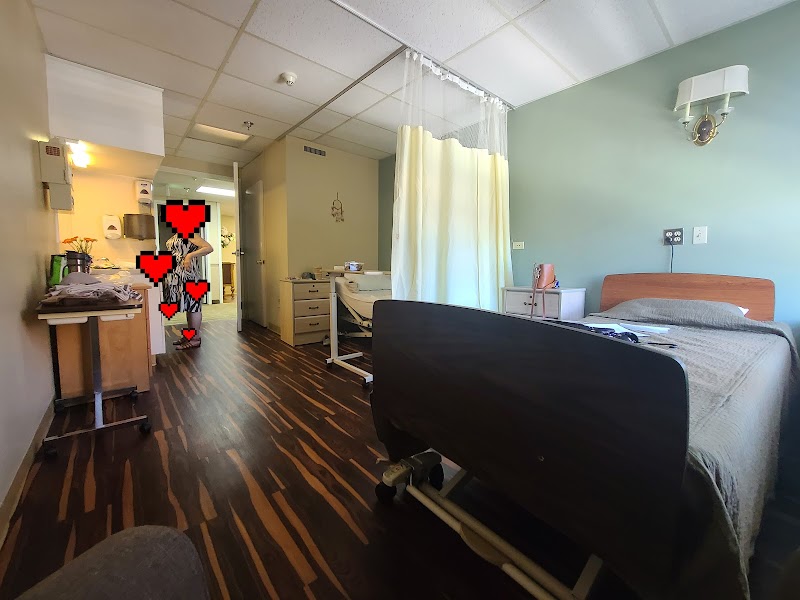



Photos powered by Google
BRIARWOOD HEALTH CARE CENTER
1440 VINE ST, DENVER, CO 80206
201 beds · For profit - Corporation Wheelchair accessible
CMS Provider #065255
Data updated: April 1, 2026
Visiting hours
- Monday: Open 24 hours
- Tuesday: Open 24 hours
- Wednesday: Open 24 hours
- Thursday: Open 24 hours
- Friday: Open 24 hours
- Saturday: Open 24 hours
- Sunday: Open 24 hours
Overall Rating
★★★★★
Health Rating
★★★★★
Staffing Rating
★★★★★
Quality Rating
★★★★★
Daily nursing care
3.9 hrs/resident
Steady
Inspection findings
5
Fewer issues
Ownership changes
0
Owned by Life Care Centers of America; single individual holds 100% ownership.
Complaint trend
Steady
One complaint-related inspection finding in the most recent cycle.
Facility vs. Colorado Averages
Overall Rating
Health Inspection
Staffing Rating
Quality Rating
BRIARWOOD HEALTH CARE CENTER — Overview
Briarwood Health Care Center is characterized by high staff retention and zero reliance on agency labor, though records show recent financial penalties for medication errors and a reduction in nursing hours during weekend shifts.
Located at 1440 VINE ST, DENVER, CO 80206. 201-bed for profit - corporation nursing facility with a CMS overall rating of 4 out of 5 stars. Google reviewers rate it 4.4 out of 5 across 165 reviews.
Unlock the Full Report
- NursingHomeIQ Score & AI Analysis
- Performance Trends Over Time
- Staffing Deep Dive
- Google Reviews & Ratings
- Inspection & Deficiency History
- Penalties & Fines
- Ownership History & Details
- Neighborhood & Location Data
- Downloadable PDF Report
Sign in to purchase or use existing credits.
Single reports are yours forever. The 30-report pass is valid for 30 days.
Data updated: April 1, 2026 · CMS, OSCAR, state inspection records
NursingHomeIQ provides informational synthesis to help families make informed decisions. This does not constitute legal, financial, or medical advice.
We use cookies for anonymous analytics to improve the site. No ads, no tracking across sites. Privacy Policy